|
 Table 1 – Human fatalities from marine animal envenomation. Table 1 – Human fatalities from marine animal envenomation.
|
Geographical locations – Human fatalities from marine envenomation
|
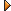 |
Blue-ringed octopus
Australia, Singapore
|
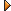 |
Cone Shell
Australia, Fiji, India (Banda), New Caledonia, Okinawa (Japan), Vanuatu
|
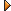 |
Sea snakes
Burma, Malaysia, India (Madras), Java (Indonesia), Okinawa (Japan), Oman, Sri Lanka, Vietnam
|
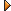 |
Stingray
Australia, California, Colombia, Fiji, New Zealand, Surinam, Texas
|
 |
Stonefish
Australia (Thursday Is.), East Africa, Japan, Seychelles
|
 BLUE-RINGED OCTOPUS BLUE-RINGED OCTOPUS
Distribution
Indo-West-Pacific – north to Okinawa, east to Philippines, west to India and south to New Zealand (including all of Australia).
Appearance
May grow to 15-20cm. in diameter with tentacles extended. Usually yellowish-brown but when irritated, many small electric-blue rings appear, making it look very attractive.
Envenomation
Minor bite from beak underneath body (often painless). The venom is ducted to the beak from the salivary glands.
Numbness of the lips and tongue may occur within minutes. In serious envenomation weakness and breathing difficulty develops rapidly, which, if untreated will develop into respiratory failure.
Fatalities
There have been two fatalities in Australia, and one in Singapore.
Medical treatment
Assisted ventilation for 4-6 hours, or possibly up to 12 hours – after which spontaneous breathing usually recurs.
NOTE: the person remains aware and conscious during this time, despite needing expired air resuscitation, or mechanical ventilation.
 SEA SNAKES SEA SNAKES
Distribution
All Oceans except for Atlantic: more common in tropical and sub-tropical zones. They may reach the upper reaches of rivers, long distances from the sea.1
Appearance
Similar to land snakes except they have flattened oar-like tail. Unlike eels, they have no gills.
Envenomation
Most bites are “dry” – less than 10% of sea snakes actually inject any venom. The bite is relatively painless, and if venom is injected, is followed by symptoms including drowsiness, nausea and vomiting, weakness, visual disturbances, breathing problems and muscle pains or stiffness. Myolysis may cause renal impairment.
Fatalities
Hundreds of fatalities from sea snake envenomation have occurred in the Countries listed in Table 8. Current estimates of the fatality rates worldwide are around 3 per cent – at least 150 deaths annually (Prof. David Warrell, pers. com. 1997).
Medical treatment
Intravenous antivenom, as needed. However, the role of antivenom in reducing the extent of myolysis is at present uncertain. . Other measures in the management of myolysis include good hydration and the maintenance of a good urinary output. Renal failure should be treated along standard lines. Primary coagulopathy does not occur in sea snake envenomation.
NOTE: Tiger snake antivenom can be used if sea snake antivenom is unobtainable.
Care of the airway and breathing in the usual way (intubation and ventilation). Any patient suspected of being envenomed by a sea snake should be observed for 24 hours following the cessation of the appropriate first aid measures.1 Tetanus immunisation should be considered. Follow-up to exclude secondary infection may be necessary.
 CONE SHELL CONE SHELL
Distribution
Indian and Pacific Oceans east to Hawaii, north to Okinawa, Japan, and south to New Zealand (including the whole of Australia).
Appearance
A cone shape with a slit-like aperture running the full length of the shell, which may be up to 15cm in length (Figure 2).
Envenomation
Pain at the site of envenomation, occasionally mild, occasionally severe and excruciating. The envenomated area may blanch, or develop a bluish tinge, and is followed by numbness and local swelling.
In serious envenomations incoordination and muscular weakness may develop rapidly, and swallowing, speech, vision and hearing may be affected. Nausea, generalised pruritus and respiratory paralysis may develop.
Fatalities
Up to 15 deaths have been claimed in Countries listed in Table 8, but the exact number is uncertain. Conus geographus is responsible for the majority of confirmed deaths, with Conus textile responsible for one death and suspected in one other.1 Recently two deaths in Japan (from Conus geographus) have occurred (Kohama 1997, pers. com.).
Medical treatment
There is no specific treatment, and symptoms and signs should be treated under the usual guidelines.1 As with any envenomation, marine or otherwise tetanus immunisation is advised and follow-up to exclude secondary infection may be necessary.
 STINGRAY STINGRAY
Distribution
Worldwide tropical and sub-tropical waters. Their main contact area with humans is in very shallow water.
Appearance
Large flat-shaped fish having a whip-like tail.
Envenomation
Stingrays often burrow under the sand in shallow water. The usual method of injury is a reflex forward whip of the tail when the `wings’ are trodden on. The tail contains one or more sharp barbs, which may embed in the skin of the victim and break off, or glance across the skin causing a laceration, which may be quite deep and extensive.
The wound is usually (though not always) acutely painful. Most occur on the lower limbs but there have now been two deaths in Australia after the barb penetrated the heart. Other serious injuries have also occurred after the barb penetrated the chest or abdomen.
Fatalities
At least 17 fatalities from stingrays have occurred worldwide, including New Zealand, Surinam, West Atlantic, Texas,23 Fiji, California,24 Australia, and many more from a fresh-water species in Colombia.1 Trunk wounds cause most of the fatalities, but acute exsanguination has caused at least two, and one death occurred from tetanus complicating a lower leg wound.1
Medical treatment
The barb sheath ruptured on penetration of the affected area, leaving tissue and venom, which will cause necrosis and infection. The whole tract is excised, if possible, and the crater packed with an alginate-based wick to allow healing by secondary intention. These dressings are useful in toxin absorption and are left in place for as long as possible. They frequently fall out at about 8-10 days, or are then easily removed without pain or damage to the healing wound. Tetanus immunisation is advised. Follow-up to exclude secondary infection may be necessary.
Wounds to the chest or abdomen MUST be carefully evaluated early, by a skilled medical team with advanced imaging.
 STONEFISH STONEFISH
Distribution
Indian and Pacific Oceans north to China, east to Hawaii and south to Australia.
Appearance
A true fish 20-30 cms long. It has tough, warty skin, which may be covered with slime (Figure 4). It is usually the colour of its surrounds (frequent-ly dark brown). Along the back of the fish are 13 spines, which when stepped on, penetrate the skin of the victim injecting venom.
Envenomation
Immediate, severe pain which may cause the patient to become frantic, or delirious. Often bluish discolouration is present around the puncture site. The area surrounding is usually oedematous (Figure 5). Local limb paralysis, nausea and vomiting, faintness may occur.
Fatalities
Deaths from stonefish envenomation are rare. They are also difficult to actually confirm, with just five deaths reported. Three are documented, but difficult to prove conclusively: one at Mahé, Seychelles, and the other at Pinda, Mozambique and a third reported recently, when a SCUBA diver stepped on a stonefish underwater, panicked, and then ascended too rapidly, death occurring from arterial embolism, not envenomation (Kohama 1997, pers. com.). A death was reported from Japan prior to 1989 of a male trying to put a stonefish in a bag. He had four puncture marks and “fell down and was drowned”. Another death was reported to have occurred on Thursday Island in 1915, several days’ following envenomation, although the author believes the causative animal is in doubt.
Medical treatment
Parenteral opioids are usually necessary; local anaesthetic (without adrenaline) or, preferably, local nerve block. Tetanus immunisation is advised. Follow-up to exclude secondary infection may be necessary.
Antivenom is available for intractable pain, or systemic symptoms.
|